Stop Overdose Stokes (S.O.S.) is a team of professionals, pastors and volunteers that formed in January of 2019 to engage churches to help reduce overdoses in Stokes County.
We meet second Wednesday of the month at 1:30pm in the fellowship hall of Chestnut Grove UMC. Address is 1024 Volunteer Rd, King and Rev. Dr. Evelyn Lemons chairs this group. Contact her at the church office at 336-983-9657 or by email at evelyn.lemons@gmail.com.

If you are a faith leader and would like more information related to substance use issues that may affect your congregation click on the links below.
Rural Faith Leaders Workshop Series: Empowering Faith Leaders to Help Persons with Substance Use Disorder

SUBSTANCE USE RESOURCE GUIDE FOR FAITH LEADERS
Alcohol is the most widely used substance due to it’s high availability. Youth who wait until they are 21 to have their first drink are four times less likely to develop alcohol-dependency.
-
Alcohol use: Youth and adults
- What is binge drinking?
- Information related to underage drinking.
- Information related to alcohol use by women.
- Information about Fetal Alcohol Spectrum Disorders.
- Information related to alcohol use in college.
- How to talk to youth about alcohol use
- Encourage parents of high school youth to talk about about celebrating safely
- Parenting support to prevent childhood alcohol use
- Share the pledge to stop underage drinking
- Alcohol facts and figures: Estimated 95,000 men and women die nationally from alcohol-related causes.
- Understanding Alcohol Use Disorder.
- Alcohol’s effects on the body.
-
Marijuana Use: youth and adults
- Marijuana is the most commonly used psychotropic drug in the United States, after alcohol. Learn about the use of marijuana in the U.S.
- What is marijuana?
- Over 10% of 8th graders, more than 22% of 10th graders and almost 28% of 12th graders have reported vaping marijuana at some point.
- Learn the real facts about how marijuana can impact teenagers.
- What are marijuana concentrates, and what do caregivers of youth need to know?
-
over-the-counter cough syrup Misuse
- Stanford University report on cough syrup misuse by teens.
- What is DXM and what do you need to know about it?
- Teen slang terms for misusing cough syrup that every caregiver of youth should know.
- Missing cough medicine could be a sign of misuse.
- Encourage parents to make sure they are checking labels of over-the-counter medicines.
-
Prescription medication misuse
- Learn about CNS (central nervous system) medications and why they should be secured properly at all times.
- Learn more about prescription opioids and how accidental misuse of opioids can happen to any family. Don’t take medication storage lightly, make sure all prescriptions are securely stored.
- Some people take prescription stimulants to try to improve mental performance. Learn how this is dangerous for teens AND adults to help prevent negative health outcomes.
-
prescription opioids and heroin research
- Prescription opioid use is a risk factor for heroin use.
- Prescription opioids and heroin have similar effects but different risk factors.
- Increased drug availability is associated with increased use and overdose.
- Heroin use is driven by its low cost and high availability.
- Emphasis is needed on both PREVENTION and TREATMENT.




 Parents and adult caregivers need to be educated about this problem, as well as their role in preventing it.
Parents and adult caregivers need to be educated about this problem, as well as their role in preventing it.




 Kratom: What are the health effects?
Kratom: What are the health effects?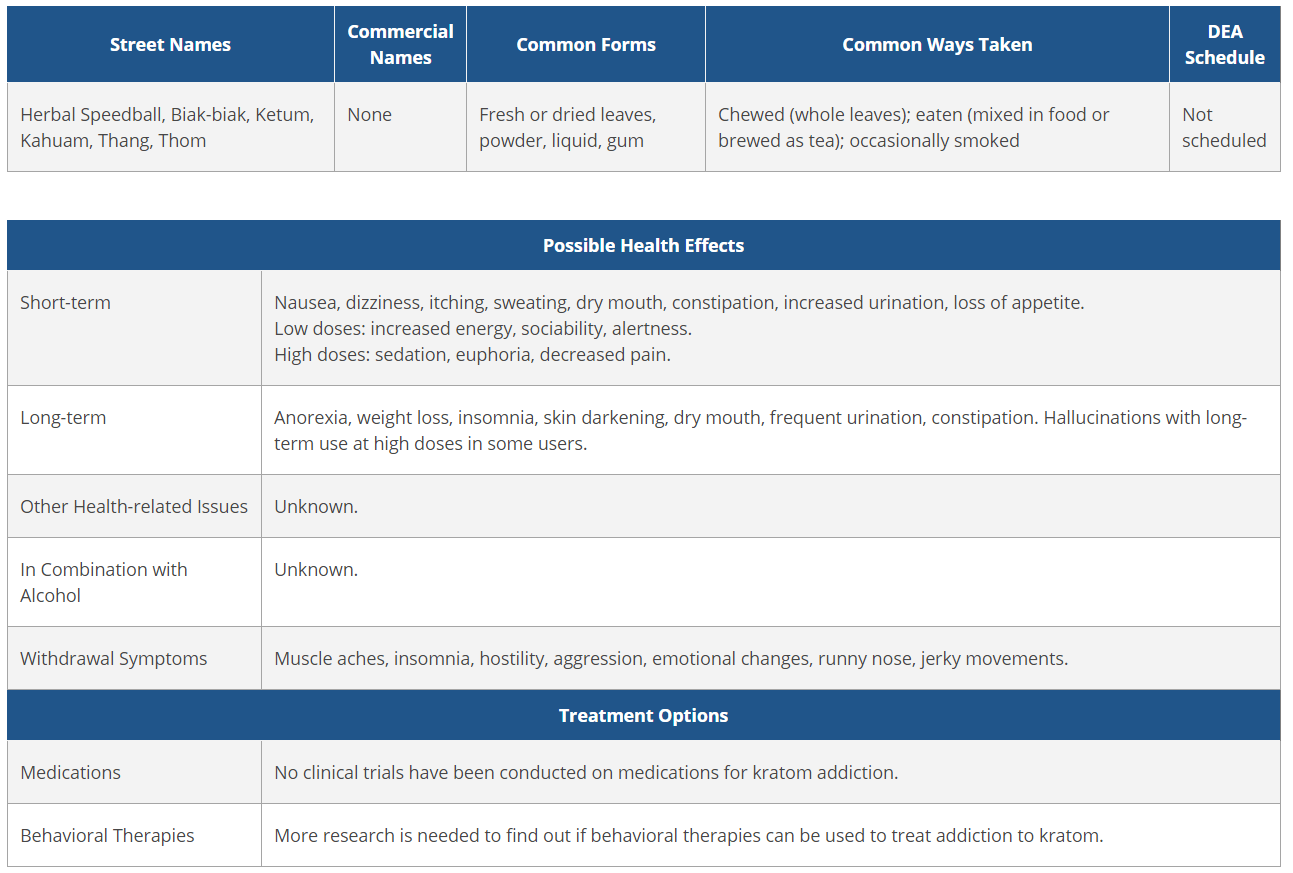



 If there is COVID-19 in your community:
If there is COVID-19 in your community: